By: Vitorio Nastasi, Policy Analyst, Reason Foundation; Adjunct Scholar, The James Madison Institute
Click here to read the full PDF of “Protecting Florida’s Most Vulnerable: Market-Based Reform to Improve Nursing Home Care”
1. Introduction
The COVID-19 pandemic has highlighted significant shortcomings in our healthcare system and, perhaps most particularly, in the nursing home industry. Strikingly, nursing home residents represent six percent of cases and 40 percent of fatalities nationwide. In Florida alone, more than 7,700 nursing home residents have died from COVID-19––about 40 percent of the state’s total fatalities.[1]
The tragedy unfolding in Florida’s nursing homes is a consequence of long-standing failures in the industry nationwide. A recent report from the federal Government Accountability Office found that infection control problems were widespread before the pandemic.[2] In fact, infection control was the most common deficiency identified through regular inspections conducted by state survey agencies. Between 2013 and 2017, 82 percent of all facilities surveyed––and 87 percent of those surveyed in Florida––had an infection control deficiency in one or more years.[3]
The problem isn’t limited to infection control. In 2019 alone, a staggering 95 percent of facilities in Florida were cited with at least one violation of the Centers for Medicare and Medicaid Services’ (CMS) quality standards.[4] Large percentages of Florida’s nursing homes had violations across a variety of categories including food sanitation, personnel qualifications, and inappropriate use of drugs (FIGURE 1).[5]
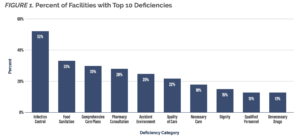
Source: Kaiser Family Foundation’s State Health Facts
Ensuring the quality and affordability of nursing home care is especially important in Florida, where more than 20 percent of the population is over 65 years old. Today, Florida has approximately 700 licensed nursing homes caring for over 70,000 residents.[1] That makes Florida home to the 6th highest number of nursing home residents in the nation. The demand for nursing home care is likely to increase as the share of the population over 65 years old is projected to climb to 1 in 4 Floridians by 2035.[2] The population over 85 years old will more than double by 2040 (FIGURE 2).
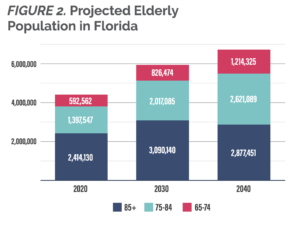
Source: Florida Office of Economic and Demographic Research
As Florida’s elderly population continues to grow, the Sunshine State has a tremendous opportunity to become a national leader in the transformation of nursing home care. The remainder of this policy study outlines obstacles to, and opportunities for, the improvement of nursing home care in Florida. Section 2 explains respective roles of regulation, competition, and consumer access to information in improving nursing home quality. Section 3 describes the effects of Certificate of Need laws on costs, quality, and competition. Section 4 discusses promising innovations in the nursing home industry and potential policy barriers to their implementation. Finally, Section 5 provides recommendations for reform.

Endnotes:
[1] “Total Number of Residents in Certified Nursing Facilities,” Kaiser Family Foundation. https://www.kff.org/other/state-indicator/number-of-nursing-facility-residents/?currentTimeframe=0&sortModel=%7B%22colId%22:%22Location%22,%22sort%22:%22asc%22%7D
[2] “Population Projections By Age, Sex, Race, And Hispanic Origin For Florida And Its Counties, 2020–2045, With Estimates For 2019,” Bureau of Economic and Business Research, 2020. https://www.bebr.ufl.edu/population/population-data/population-projections-age-sex-race-and-hispanic-origin-florida-and-its-4
[1] As of 12/14/2020. “State Data and Policy Actions to Address Coronavirus,” Kaiser Family Foundation, 2020. (Accessed 17 Dec. 2020). https://www.kff.org/health-costs/issue-brief/state-data-and-policy-actions-to-address-coronavirus/#long-term-care-cases-deaths
[2] “Infection Control Deficiencies Were Widespread and Persistent in Nursing Homes Prior to COVID-19 Pandemic,” Government Accountability Office, GAO.gov, 20 May 2020. https://www.gao.gov/assets/710/707069.pdf
[3] Ibid.
[4] “Percent of Certified Nursing Facilities with Deficiencies,” Kaiser Family Foundation. https://www.kff.org/other/state-indicator/nursing-facilites-with-zero-deficiencies/?activeTab=map¤tTimeframe=0&selectedDistributions=percent-with-deficiencies&sortModel=%7B%22colId%22:%22Location%22,%22sort%22:%22asc%22%7D
[5] “Percent of Certified Nursing Facilities with Top 10 Deficiencies,” Kaiser Family Foundation.











